太ももやお尻の脂肪を手軽に落とすなら脂肪溶解注射
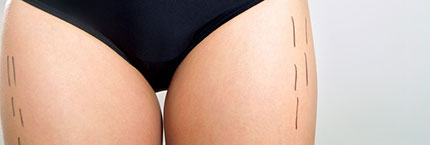
痩せたい部分は人それぞれ違いがありますが、太ももやお尻や特に脂肪がつきやすく悩んでいる人は多いのではないでしょうか!?
綺麗なスタイルにするためには、食事制限やエクササイズなどで努力することも大事ですが、一般的なダイエットでは、部分的に脂肪を落とすことは難しく、バストなど落ちてほしくない部分もサイズダウンする傾向にあります。そして、理想のスタイルになるまでには時間もかかりますので、運動や食事制限が続かないと悩む人もいます。

即効性を期待するのであれば、美容医療を取り入れることも考えてみましょう。

部分痩せ治療では脂肪吸引が有名ですが、体に傷が残ることやダウンタイムが長いことで抵抗を持つ人も少なくありません。より楽に、自然な痩身を得るのであれば脂肪溶解注射も考えてみましょう。これは、脂肪を溶かしやすくする薬剤を気になる部分に注入することで、部分痩せを目指す治療です。溶けだした脂肪は血管を通り、尿や汗と一緒に排出されていきます。通常のダイエットでは脂肪細胞は小さくなるものの、数を減らすことができないので、リバウンドしやすい傾向にあります。その点、脂肪溶解注射なら脂肪細胞の数を減らすこともできますので、リバウンドしにくいこともメリットです。

厳しい食事制限の必要もなく、運動をすることもなく痩せることができますので、ダイエットが長続きしない人にも効果的です。
美容皮膚科などでの施術というと、時間がかかるイメージもありますが、注射だけなので短時間の施術で済みます。すぐに普通の生活に戻ることができますので、ダウンタイムの心配もほとんどありません。
気になる部分の脂肪を減らせることはもちろん、セルライト除去の治療としても注目されています。
都会の場合、地方都市とは違い多数の美容皮膚科があり、どこで脂肪溶解注射をしたらいいのか迷うことでしょう。何回もカウンセリングに行けばいいのですが、時間がかかり忙しい方はいけません。
大坂の心斎橋や福岡の博多などで脂肪溶解注射を希望している方は、下記のサクラアズクリニックを検討してみてください。医師や看護師の多くが女性なのでおすすめです。
脂肪溶解注射(メソセラピー) | 大阪心斎橋/京橋・福岡天神[サクラアズクリニック]
価格や施術の流れなど、チェックしてください。

目の周囲にしわやたるみがある場合はフラクショナルアイリフト

目の周囲にしわやたるみがあると、実年齢よりも老けた印象を与えます。しかし、目の周囲は皮膚が薄いので、手術を受けることに抵抗がある方もいます。しわやたるみの悩みを解決したいなら、美容皮膚科で相談しましょう。美容皮膚科では、フラクショナルアイリフトによる治療を行っています。
フラクショナルアイリフトとは、目の周囲にできたしわやたるみを医療用レーザーによって改善する施術です。しかも、微細なレーザーで表面に穴を開けて、肌に刺激を与えます。本来、肌が持っている再生能力を引き出すところが、フラクショナルアイリフトの特徴です。

フラクショナルアイリフトの施術を受けることによって、コラーゲンの生成を促進します。その結果、目の周囲に弾力のある肌を再生することができます。肌が引き締まりますので、しわやたるみの症状を改善します。フラクショナルアイリフトの施術を受けたいなら、美容皮膚科でカウンセリングを申し込みましょう。美容皮膚科のホームページから入力することも可能です。カウンセリングは無料ですし、詳しい説明を受けられます。料金に関する質問も受け付けています。
フラクショナルアイリフトの施術を受ける前に、麻酔クリームを塗ります。施術にかかる時間は10分から20分程度ですが、症状によって異なります。尚、一回の施術で効果が出ないケースもあります。定期的に通院する場合は、1か月から2か月程度の間隔を開けましょう。
施術を受けた後に、肌が赤くなる方もいます。赤みが消えるまで、帽子やサングラスで隠しましょう。患部に紫外線が当たるのを避けることもできます。

